safetrach™

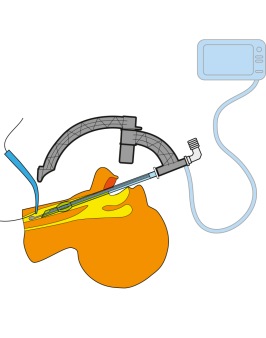
Percutaneous tracheotomy set is successfully used all over the world. The technique has many advantages but still have a few draw-backs. One problem is to properly identify the correct place for tracheotomy and an other is the safety concern of making the puncture in the midline of the anterior wall of the trachea and not damaging the posterior wall. The technique also requires two physicians well trained in the technique, one actually performing the tracheotomy, and one supervising the other through a fibre bronchoscope.
SafeTrach, which is based on the company's patented tweezers concept, is suitable in the intensive care unit as well as in the ENT unit. SafeTrach demands much less efforts from the anaesthesiologist’s point of view.
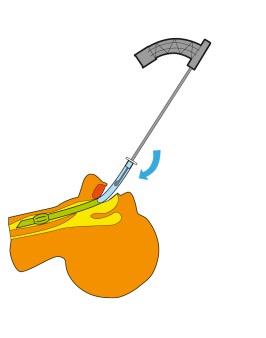
With SafeTrach, the inner shaft is introduced through the orotracheal tube. To introduce something through the orotracheal tube is very common both for doctors and nurses.
It is very common to suck through the orotracheal tube in order to clean trachea. So, to introduce the SafeTrach inner shaft through the orotracheal tube is easy for the staff as well in the intensive care unit as in the ENT unit. There is no risk to harm the larynx and you do not need any laryngoscopic control.
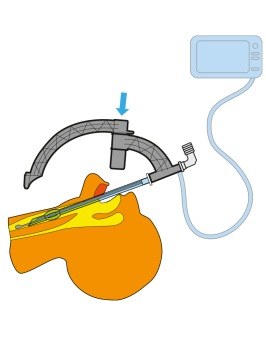
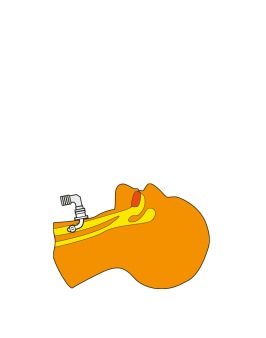
After the introduction of the inner shaft, the outer shaft is connected and then you have very good opportunity to do the penetration in such way that you always will penetrate in the midline of trachea. Furthermore, there are inbuilt protectors
guaranteeing that it is impossible to harm the posterior tracheal wall.
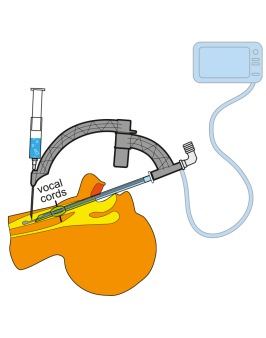
During the procedure you have total control of the level of penetration in relation to the vocal cords and there is no risk of accidental extubation as you can check where you are using the outer shaft that shows where the inner shaft is located.
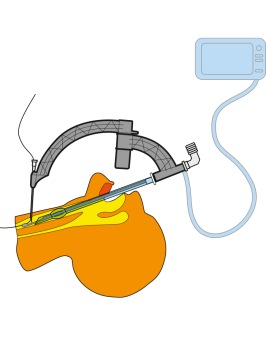
During the total procedure you ventilate the patient through the SafeTrach inner shaft, eliminating the risks and uncertainties involved when you do the procedure with a bronchoscope through the orotracheal tube that limit the lumen for ventilation.
Another big advantage is when you use a percutaneous tracheotomy set, and we mean whatever percutaneous set there is available on the market, (except from Fantoni technique) the dilation means that the trachea will be compressed from the outside. However, with help of the inner shaft the tracheal wall can be tilted outwards which can support and ease the dilation.
- Safe puncture in the midline of the anterior wall of the trachea at the right level without need for simultaneous fibre bronchoscopy
- No risk of hurting the posterior wall of the trachea
- In consequence, the procedure needs only one physician, even with limited experience, with improved safety compared to current percutaneous tracheotomy techniques.
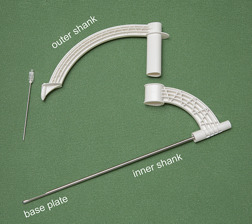
SafeTrach consists of the following parts:
•An inner shank inserted in an orotracheal tube
•A fiberoptic scope inserted in the inner shank
•An outer shank connected to the inner shank
•A puncturing needle attached to the outer shank
ADVANTAGES USING SAFETRACH
FOR PATIENTS
- Safer procedure (Traditional PT experience complications in 1 out of 10 procedures)
- Ventilation secured during operation
- Shorter surgical procedure (Traditional PT approx 30 min. SafeTrach approx 15 min)
FOR DOCTORS
- Short learning curve (Traditional PT approx. 30 procedures needed)
- Technique based on traditional skills
- Shorter surgical procedure
FOR HOSPITALS
- Less staff intensive (1 doctor compared with traditionally 2)
- Time saving
- Decreased product costs
- Increased patient capacity with reduced patient stay at ICU (3-5 days with an early tracheotomy)